Chemical Properties
White Solid
Usage
A novel antithrombotic agent. A highly potent and selective, direct FXa inhibitor
Usage
anti-coagulant, Factor X inhibitor
Originator
Bayer (Germany)
Definition
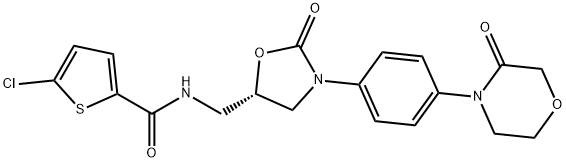
ChEBI: A monocarboxylic acid amide obtained by formal condensation of the carboxy group of 5-chlorothiophene-2-carboxylic acid with the amino group of 4-{4-[(5S)-5-(aminomethyl)-2-oxo-1,3-oxazolidin-3-yl]phenyl}morpholin-3-one. An anticoagulant u
ed for prophylaxis of venous thromboembolism in patients with knee or hip replacement surgery.
Pharmacokinetics
Rivaroxaban(366789-02-8) was absorbed rapidly with maximum plasma concentrations (Cmax) being reached 2–4 h after a single dose (1.25–80 mg) and multiple doses (up to 30 mg twice daily). Rivaroxaban did not accumulate to a relevant extent after multiple dosing. Data from phase I studies in healthy subjects showed that absorption is almost complete (oral bioavailability approached 80–100 %) for the 10 mg tablet dose, irrespective of fasting or fed conditions[3]. When administered orally with food, AUC and Cmax values were similar for whole and crushed rivaroxaban 20 mg tablets, whereas a crushed tablet suspended in water, administered using a nasogastric tube and followed by a liquid meal, gave similar AUC values but an 18 % reduction in Cmax.
Clinical Use
Factor Xa inhibitor:
Prevention of venous thromboembolism in adult
patients undergoing elective hip or knee replacement
surgery
Treatment of DVT or PE
Prophylaxis of stroke in AF
Prophylaxis of atherothrombotic events in ACS
Side effects
Regarding safety, there was no statistical difference in the incidence of major postoperative bleeding between any of the rivaroxaban dose groups and enoxaparin although there did appear to be a dose dependency in the rivaroxaban set. In addition to bleeding and subsequent posthemorrhagic anemia, presenting as weakness, paleness, asthenia, dizziness, headache, or unexplained swelling, other common adverse events included nausea, increased GGT, and an increase in transglutaminase. Owing to its mechanism of action, there is a bleeding risk, so the drug is contraindicated in patients with clinically active bleeding. Rivaroxaban is also contraindicated in pregnant and breast-feeding women and in patients with hepatic disease associated with coagulopathy and clinically relevant bleeding risk.
Synthesis
Rivaroxaban(366789-02-8) is a recent market introduction that directly inhibits FXa with high potency (Ki 0.4 nM; IC50 0.7 nM) and selectivity, W10,000-fold over other related serine proteases (thrombin, trypsin, plasmin, FVIIa, FIXa, FXIa, urokinase, and activated protein C). From the X-ray crystal structure, the central oxazolidinone moiety anchors the drug through two hydrogen bonds to Gly219 and directs the morpholinone group into the S4 pocket and the chlorothiophene portion into the S1 pocket. These key components may be coupled together synthetically by a couple of routes. Condensation of 3-morpholinone with 4-fluoronitrobenzene followed by catalytic hydrogenation provides N-(p-aminophenyl)morpholinone for subsequent reaction with (S)-2-(phthalimidomethyl)oxirane. With establishment of the aminoalcohol adduct, cyclization with 1,1 -carbonyldiimidazole generates the central oxazolidinone. Deprotection and acylation with 5-chlorothiophene-2-carbonyl chloride affords rivaroxaban. The drug is formulated in 10-mg tablets for once-daily oral administration to patients undergoing elective hip or knee replacement surgery to prevent VTE.
Drug interactions
Potentially hazardous interactions with other drugs
Analgesics: increased risk of haemorrhage with IV
diclofenac and ketorolac - avoid.
Antibacterials: concentration reduced by rifampicin.
Anticoagulants: increased risk of haemorrhage with
other anticoagulants - avoid.
Antidepressants: concentration possibly reduced by
St John's wort.
Antiepileptics: concentration possibly reduced
by carbamazepine, fosphenytoin, phenobarbital,
phenytoin and primidone.
Antifungals: concentration increased by ketoconazole
- avoid; avoid with itraconazole, posaconazole and
voriconazole.
Antivirals: avoid with atazanavir, darunavir,
fosamprenavir, indinavir, lopinavir, saquinavir and
tipranavir; avoid with lopinavir; concentration
increased by ritonavir - avoid.
Cobicistat: possibly enhanced effect with cobicistat
- avoid.
Metabolism
Metabolised by the cytochrome P450 isoenzymes
CYP3A4 and CYP2J2 and by other mechanisms.
About two-thirds of an oral dose is metabolised, with
the metabolites excreted equally in the urine and faeces;
the remaining third is excreted unchanged in the urine,
mainly by active renal secretion.
Mode of action
Rivaroxaban(366789-02-8) is a direct, specific Factor Xa inhibitor. In vitro kinetic studies showed that the inhibition of human Factor Xa by rivaroxaban was competitive [inhibition constant (K i) 0.4 ± 0.02 nM] with 10,000-fold greater selectivity than for other serine proteases—it does not inhibit related serine proteases at concentrations up to 20 μM. This compound potently inhibited prothrombinase activity [inhibitory concentration 50 % (IC50) 2.1 ± 0.4 nM], and clot-associated Factor Xa activity (IC50 75 nM). In human plasma, rivaroxaban inhibited endogenous Factor Xa activity in a concentration-dependent manner with an IC50 of 21 ± 1 nM [19]. In an ex vivo study, rivaroxaban at a single dose of 5 mg and 30 mg reduced collagen-induced endogenous thrombin potential in human plasma by approximately 80 and 90 %, respectively, and tissue factor-induced endogenous thrombin potential by approximately 40 and 65 %, respectively. In contrast to indirect Factor Xa inhibitors, rivaroxaban does not require any cofactor to exert its anticoagulant effect. In human plasma, rivaroxaban concentration-dependently inhibited thrombin generation and, thus, the amplification processes of coagulation. Thrombin generation was almost completely inhibited at therapeutically relevant concentrations (80–100 nM) of rivaroxaban. In addition, rivaroxaban increased the permeability and degradability of the whole blood clot, by decreasing thrombin generation. However, rivaroxaban does not inhibit the activity of pre-existing thrombin molecules[1-2].
References
[1] Mueck, W., et al. "Clinical Pharmacokinetic and Pharmacodynamic Profile of Rivaroxaban."Springer Open Choice 53(2014):1-16.
[2] Perzborn, E., et al. "In vitro and in vivo studies of the novel antithrombotic agent BAY 59-7939—an oral, direct Factor Xa inhibitor." Journal of Thrombosis and Haemostasis 3.3(2005):514-521.
[3] Kubitza, Dagmar , et al. "Safety, pharmacodynamics, and pharmacokinetics of BAY 59-7939—an oral, direct Factor Xa inhibitor—after multiple dosing in healthy male subjects." European Journal of Clinical Pharmacology 61.12(2005):873-80.