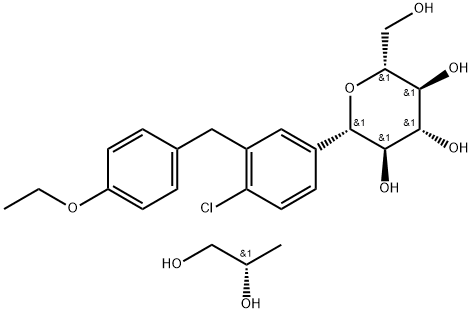
Dapagliflozin Propanediol Monohydrate: Safety & Clinical Application
Dapagliflozin propanediol monohydrate is a sodium-glucose co-transporter-2 (SGLT2) inhibitor used to treat type 2 diabetes, heart failure, and chronic kidney disease. By reducing glucose reabsorption in the kidney, it improves glycemic control. It also provides cardiovascular and renal protection, making it a valuable therapy in both diabetic and non-diabetic patients. Dapagliflozin Propanediol primarily functions by inhibiting the SGLT2 protein, which is located in the proximal tubule of the nephron in the kidneys. SGLT2 is responsible for reabsorbing approximately 90% of the glucose filtered by the kidneys under normal physiological conditions. Dapagliflozin propanediol monohydrate exerts protective effects on kidney function by reducing hyperfiltration and intraglomerular pressure, which are key contributors to kidney damage in both diabetic and non-diabetic CKD.

Efficacy and Safety of Dapagliflozin propanediol monohydrate
Type 2 diabetes mellitus (T2DM) is a worldwide problem that is growing in prevalence. An estimated 347 million people worldwide are diagnosed with diabetes, and 90–95% of those have T2DM. Antihyperglycemic agents with innovative mechanisms and synergistic effects when used in combination with other antihyperglycemic agents are necessary to extend the number of treatment options available to patients with T2DM. Medication adverse effects, drug–drug interactions, concurrent illnesses, and hospitalizations can all cause hyperglycemia and result in difficulty maintaining glycemic control. Current guidelines advocate for initiating lifestyle modifications and metformin as first-line therapy, but beyond that, antihyperglycemic management becomes very patient specific. Sodium-glucose cotransporter 2 (SGLT2) inhibitors are a new therapeutic class of oral agents for the treatment of T2DM. This therapeutic class currently includes three agents: canagliflozin, dapagliflozin, and empagliflozin. Dapagliflozin propanediol monohydrate was approved in the US on 8 January 2014 and has previously been approved and is used in 38 other countries, including Europe, under the trade name Forxiga (Bristol-Myers Squibb Company, Middlesex, UK). A fixed-dose combination of dapagliflozin and metformin (Xigduo [Bristol-Myers Squibb Company, Middlesex, UK]) was also recently approved in Europe [AstraZeneca, 2014a]. This review will focus on the efficacy and safety of dapagliflozin propanediol monohydrate for the treatment of T2DM.[1]
Dapagliflozin propanediol monohydrate promotes glucose filtration through the kidneys and into the urine to be eliminated from the body. To quantify the degree of glucose excretion that occurs with dapagliflozin, studies have examined 24 h glucose excretion amounts in healthy subjects as well as patients with T2DM given a range of dapagliflozin doses. Dapagliflozin doses of 20–100 mg have resulted in urinary glucose excretion of approximately 60 g over 24 h in healthy volunteers. In subjects with T2DM who received dapagliflozin doses between 2.5 and 20 mg, the 24 h glucose excretion after 1 day ranged between 38 and 77 g and after 14 days ranged between 42 and 73 g. Henry and colleagues conducted two randomized, double-blind, double-dummy, multinational studies in treatment-naïve patients with T2DM randomized to receive dapagliflozin propanediol monohydrate plus placebo, metformin XR plus placebo, or dapagliflozin plus metformin XR for a total of six study groups. Patients receiving metformin received a dose titrated to 2000 mg. At the end of 24 weeks, patients receiving combination therapy of dapagliflozin and metformin in both trials had a greater HbA1c reduction and greater reductions in mean FPG values than patients receiving monotherapy. However, dapagliflozin propanediol monohydrate monotherapy with daily doses of 5 and 10 mg produced changes in HbA1c.
Dapagliflozin propanediol monohydrate in Type 2 Diabetes
Sodium-glucose cotransporter-2 (SGLT2) inhibitors are a relatively new class of antihyperglycaemic agents (AHAs) for the treatment of type 2 diabetes (T2D). These agents reduce reabsorption of glucose in the kidneys and facilitate its excretion in the urine by inhibiting the high-capacity glucose transporter SGLT2 located in the proximal convoluted tubule, thereby lowering glucose levels independently of insulin action. This unique mechanism of action of SGLT2 inhibitors complements that of other classes of AHAs, allowing for their use as combination therapy with other AHAs, including insulin. Dapagliflozin propanediol monohydrate (Forxiga®) is one such SGLT2 inhibitor that is approved for the treatment of T2D in various countries worldwide, including the EU and USA. The pharmacological properties and clinical use of dapagliflozin in adults with T2D have been extensively reviewed previously in Drugs . This article, written from an EU perspective, focuses on recent trials, including the large DECLARE-TIMI 58 cardiovascular (CV) outcomes trial in patients with T2D with or without established cardiovascular disease (CVD). Dapagliflozin propanediol monohydrate is also available as fixed-dose dapagliflozin/metformin (Xigduo®) and dapagliflozin/saxagliptin (Qtern®) tablets.[2]
Dapagliflozin is a highly potent (inhibitory constant 0.55 nmol/L) and reversible SGLT2 inhibitor that is > 1400 times more selective for SGLT2 than SGLT1, the main transporter responsible for glucose absorption in the gut. Dapagliflozin Dapagliflozin propanediol monohydrate increased the amount of glucose excreted in the urine and improved both fasting (FPG) and post-prandial plasma glucose levels in patients with T2D. Urinary glucose excretion (glucuresis) was seen after the first dose of dapagliflozin, was continuous during the 24 h dosing interval and maintained over the course of therapy. Dapagliflozin propanediol monohydrate-induced glucuresis in patients with T2D was associated with caloric loss and a modest reduction in bodyweight, as well as mild osmotic diuresis and transient natriuresis. The loss in bodyweight with SGLT2 inhibitors is less than that calculated from calorie loss due to glucuresis, which may be because of compensatory mechanisms such as increased energy intake. Three major hypoglycaemic events were reported in the dapagliflozin group and two in the placebo group, with most events occurring in patients receiving insulin as background therapy; one event in a patient receiving dapagliflozin plus insulin and metformin resulted in discontinuation of therapy. In DECLARE-TIMI 58, major hypoglycaemic events occurred in significantly fewer dapagliflozin propanediol monohydrate than placebo recipients (0.7 vs. 1.0%; p = 0.02).
References
[1]Anderson SL. Dapagliflozin efficacy and safety: a perspective review. Ther Adv Drug Saf. 2014 Dec;5(6):242-54. doi: 10.1177/2042098614551938. PMID: 25436106; PMCID: PMC4232499.
[2]Dhillon S. Dapagliflozin: A Review in Type 2 Diabetes. Drugs. 2019 Jul;79(10):1135-1146. doi: 10.1007/s40265-019-01148-3. Erratum in: Drugs. 2019 Dec;79(18):2013. doi: 10.1007/s40265-019-01239-1. PMID: 31236801; PMCID: PMC6879440.
You may like
See also
Lastest Price from Dapagliflozin propanediol monohydrate manufacturers

US $10.00/KG2025-04-21
- CAS:
- 960404-48-2
- Min. Order:
- 1KG
- Purity:
- 99%
- Supply Ability:
- 10 mt

US $0.00-0.00/kg2025-04-21
- CAS:
- 960404-48-2
- Min. Order:
- 1kg
- Purity:
- 99%
- Supply Ability:
- 2500kg